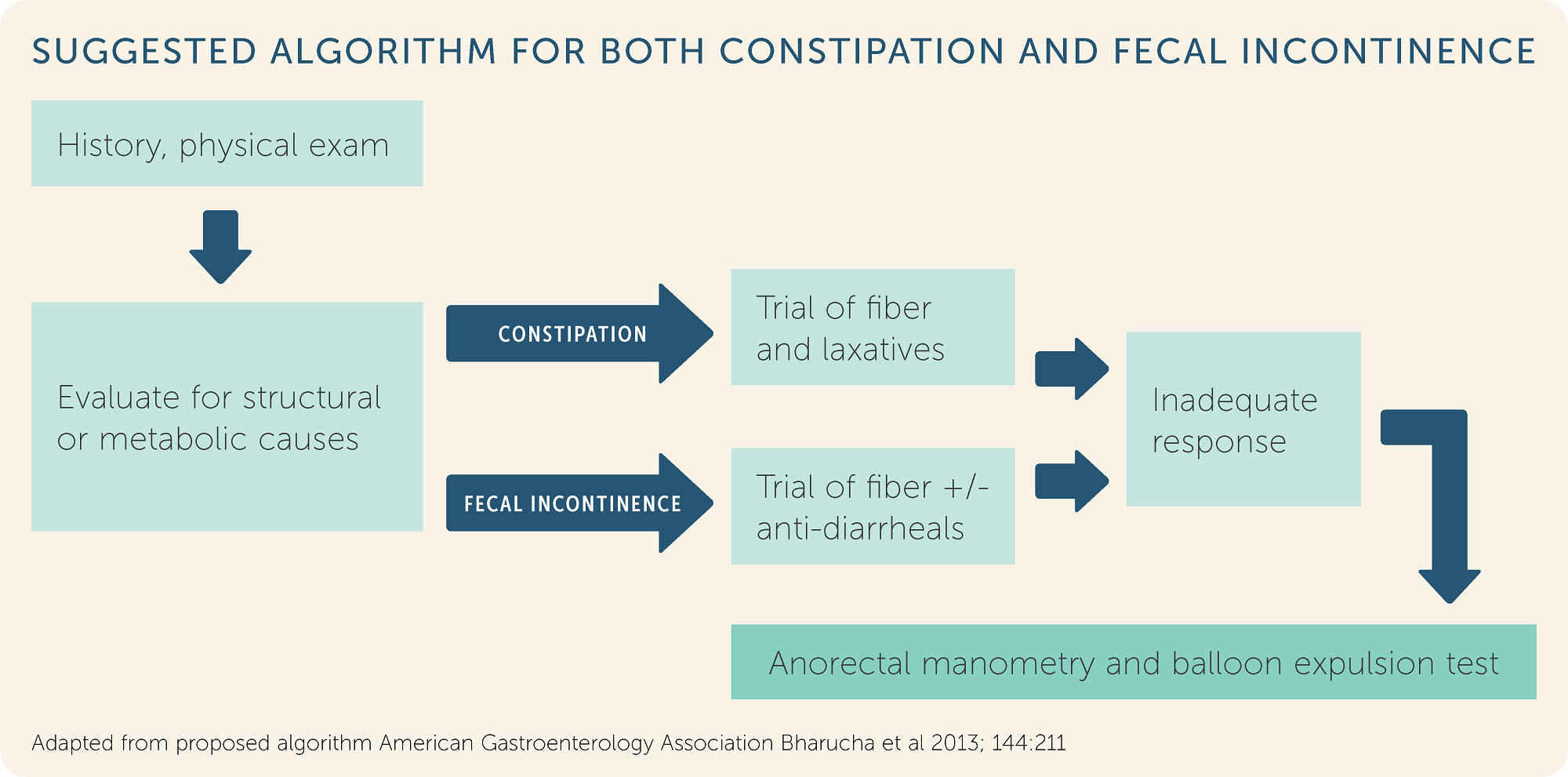
Anorectal manometry (ARM) is a study ito look further into anal sphincter and rectal pressures and function. The most common reason why we use this test is to look at constipation that isn’t responding to fiber supplementation and laxatives or when someone is having fecal incontinence.
Constipation
Some studies have suggested that up to 25 percent of people with constipation may not be coordinating their rectal muscles out (propelling stool) while at the same time relaxing their anal sphincters to allow the stool to exit effectively. When these muscles are not working in conjunction, then dyssynergic defecation occurs causing incomplete stool evacuation. Patients will describe a feeling of incomplete rectal emptying, having to strain for prolonged periods of time, needing to change positions on the toilet, using their hands to press on their abdomen or perineum/vagina or even place a finger in their rectum to get the stool to pass completely.
Anorectal manometry is done with balloon expulsion testing (BET) to evaluate constipation. The BET involves an inflatable balloon instilled with 50 cc of water placed in a patient’s rectum to see if they are able to effectively push this out within a few minutes. The ARM results provide an idea of how much rectal force is generated by patient and what kind of anal sphincter relaxation occurs during simulated defecation. ARM can also help determine if there is a problem with patients being able to sense stool in their rectum or even if there are signs consistent with irritable bowel syndrome.
Fecal Incontinence
When there is damage to nerve sensation in the rectum or the internal or external anal sphincter strength, there is a higher risk for losing stool or gas accidentally (fecal incontinence). The first step to helping patients is to ask them directly if they have fecal incontinence. Many patients feel embarrassed to bring it up, even to their medical provider. If fiber supplementation and identification and management of any underlying diarrhea problems is not enough to resolve the fecal incontinence, we can turn to anorectal manometry for further evaluation.
Anorectal manometry will help to determine if lack of sensation from nerve damage is an issue or if there is weakness in the internal or external anal sphincters. A careful physical exam and review of patient’s medical history is obtained on the day of ARM testing. Based on the results, specific recommendations are made and if it is the external anal sphincter that is weak, pelvic floor retraining with a physical therapist may help.
The Oregon Clinic Gastroenterology South offers anorectal manometry and balloon expulsion testing that can dive deeper into helping patients with constipation and fecal incontinence.
